Furthermore, the polymicrobial nature of BV 11, inability to cultivate some key BVAB 10, and lack of animal or cell culture models that fully replicate the human cervical environment and support BVAB and STI infection 42 have impeded the understanding of pathophysiological mechanisms related to BV.
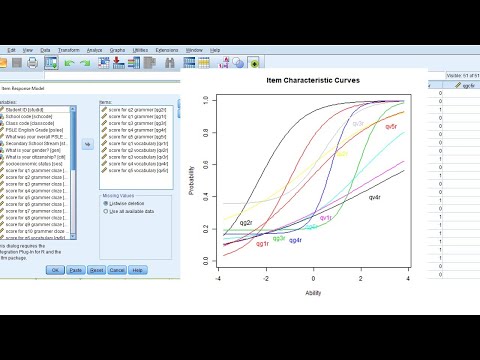
While epidemiological studies suggest that cervicovaginal microbiota are important determinants of STI susceptibility and reproductive and obstetric sequelae, they do not provide insight into how BVAB species increase the risk of STIs and result in adverse health outcomes in women. Women with BV also exhibit an increased risk of acquiring sexually transmitted infections (STIs) caused by viruses (human immunodeficiency virus (HIV) 28, 29, herpes simplex virus-2 30, 31, 32, human papillomavirus (HPV) 33, 34), bacteria ( Neisseria gonorrhoeae 35, 36, 37, Chlamydia trachomatis 35, 36, 37, Mycoplasma genitalium 38, 39) and protozoan parasites ( Trichomonas vaginalis 35, 40, 41). amnii, has been reported to cause maternal chorioamnionitis, spontaneous abortion, and stillbirth 24, 25, 26, 27. Intriguingly, the higher risk for preterm labor have been associated with high levels of particular BV-associated bacteria (BVAB), including Sneathia amnii, in vaginal fluids 20, 21, 22, 23. Multiple epidemiological studies have shown that BV is a risk factor for gynecologic, reproductive, and obstetric sequelae, such as endometritis 12, 13, pelvic inflammatory disease 14, infertility 15, 16, cervicitis 17, and preterm birth 18, 19. The etiology of this polymicrobial disorder is poorly understood 11. accompanied by an overgrowth of anaerobes, such as Gardnerella vaginalis, Prevotella bivia, Atopobium vaginae, and Sneathia spp. BV results from a depletion of these protective and health-promoting Lactobacillus spp. These beneficial bacteria protect the woman from invading pathogens by creating an acidic microenvironment via lactic acid production, secretion of antimicrobial compounds, competitive exclusion, and other mechanisms 8, 9. In healthy premenopausal women, the vagina and cervix are typically colonized by one or a few Lactobacillus species ( L. Recommended treatments for BV (metronidazole and clindamycin regimens) are also frequently ineffective in the long term, as >50% of women experience BV recurrence 4, which contributes to the high burden of disease.īV is caused by a dramatic shift in the composition of cervicovaginal microbiota 5. In clinical settings, BV is diagnosed by the Amsel criteria (thin, white vaginal discharge, presence of “clue cells” coated with bacterial biofilm, elevated pH, and malodor) 3, yet many women are asymptomatic 2. In the United States, BV affects approximately one-third of women aged 14–49 years 2. Overall, this study demonstrated that 3D cervical epithelial cell colonized with cervicovaginal microbiota faithfully reproduce the immunometabolic microenvironment previously observed in clinical studies and can successfully be used as a robust tool to evaluate host responses to commensal and pathogenic bacteria in the female reproductive tract.īacterial vaginosis (BV) is the most common vaginal infection among premenopausal women worldwide with an estimated annual economic cost of $4.8 billion 1. Alterations to the immunometabolic landscape correlate with symptoms and hallmarks of BV and connected BV with adverse women’s health outcomes. crispatus produced an antimicrobial compound, phenyllactic acid.

amnii distinctly altered physicochemical barrier-related proteins and metabolites (mucins, sialic acid, polyamines), whereas L. amnii exhibited the highest proinflammatory potential through induction of cytokines, iNOS, and oxidative stress-associated compounds. The immunometabolic profiles of these microenvironments were analyzed using multiplex immunoassays and untargeted global metabolomics. We used Lactobacillus crispatus as a representative health-associated commensal and four common BV-associated species: Gardnerella vaginalis, Prevotella bivia, Atopobium vaginae, and Sneathia amnii. Our 3D epithelial cell model that recapitulates the human cervical epithelium was infected with clinical isolates of cervicovaginal bacteria, alone or as a polymicrobial community. We hypothesized that members of the cervicovaginal microbiota distinctly contribute to immunometabolic changes in the human cervix, leading to these sequelae.
Importantly, BV is linked to adverse gynecologic and obstetric outcomes: an increased risk of sexually transmitted infections, preterm birth, and cancer. Bacterial vaginosis (BV) is an enigmatic polymicrobial condition characterized by a depletion of health-associated Lactobacillus and an overgrowth of anaerobes.
